Radical Rest and Beyond
How it went and how it's going with new treatments
I’m back!
At the end of November, I decided to go on “radical rest” in an attempt to stop the slide from moderate to severe. I feel like I did, in fact, stop the slide but I certainly did not hit remission. I’m relieved to say it expanded my baseline, but only a bit—a lot less than I thought it would. The real gains have come from some new treatments I started this spring. More on that later.
In November, I set out a schedule and plan for my radical rest. I was so optimistic. I was so sure of the plan. That was cute. Let me just say, nobody—nobody—should ever feel like they’re failing at “getting better”. Frankly, I have the tools and support needed to try radical rest and I still found so much to be out of my control or impractical. It was hard. It was really hard. My carefully designed metrics went out the window pretty quickly.
I will say, the experience was valuable, though. First, it absolutely did stabilize me when things were getting scary. Second, by combining long-term rest with the Visible tracker, I gained incredibly helpful insights into just how much energy is required for daily tasks. I came out of it with a much clearer and more accurate understanding of my pacing needs and boundaries. Not everyone can put everything on hold to prioritize total rest, but I definitely recommend trying a mini version, whatever is possible for you, if you feel like you need to stabilize and/or get a better handle on pacing.
New treatments with big improvements, you say?!?
Yes! In my previous post I included the list of treatments I was on at that time. Well, I’m changing things up a bit with the help of a new specialist and ME clinic. Before I go on…
I recognize this is an area many of us struggle with mightily. Finding a medical provider who understands and treats ME is criminally difficult. Two fully remote practices I know of our: Dr. Susan Levine (private practice) and Four Peaks Healthcare. Dr. Levine takes most insurance and files all claims on your behalf (last I checked). However, Four Peaks does not take insurance (you can file an out-of-network claim yourself, if that’s an option for you). I don’t know whether or not either practice is accepting new patients.
As for myself, I’m really benefiting from having a new set of eyes on my case. And the biggest win has been something I preach all the time. Get your comorbidities diagnosed and under control! Back in 2021, I had a tilt table test that diagnosed me with neurocardiogenic syncope/dysautonomia. At the time, the recommendation of fluids and salt felt a little weak—it felt downplayed and less pressing than other treatments. So, I didn’t weigh dysautonomia heavily in my treatment plan.
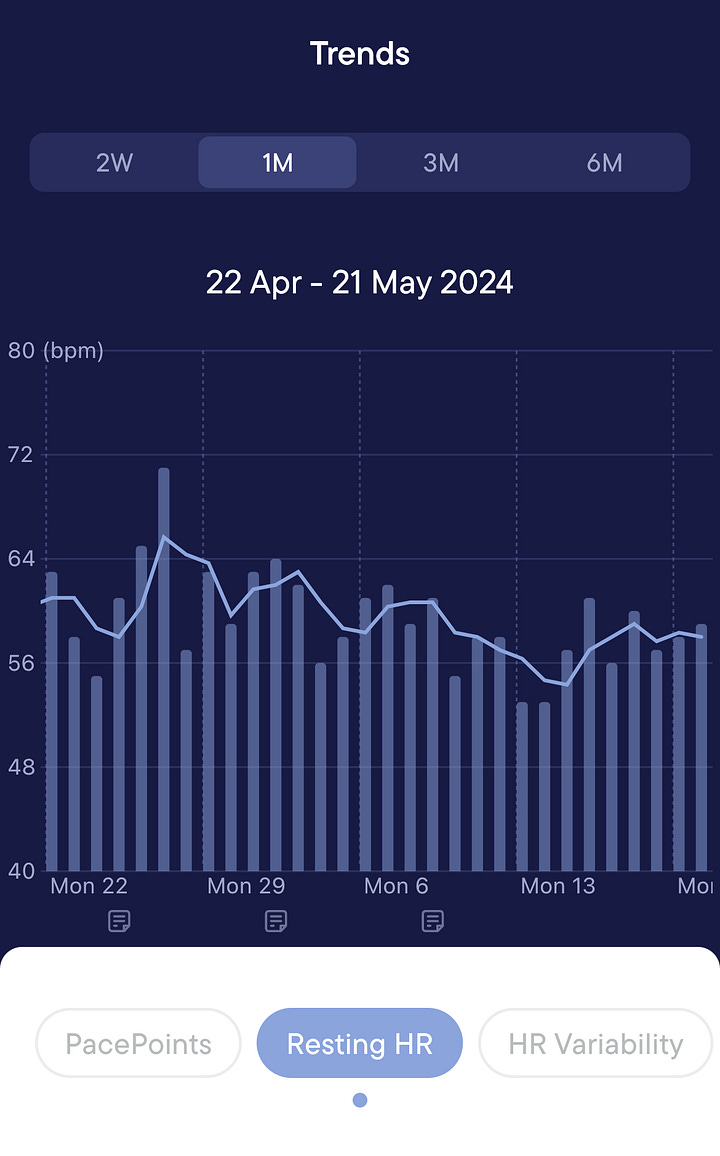
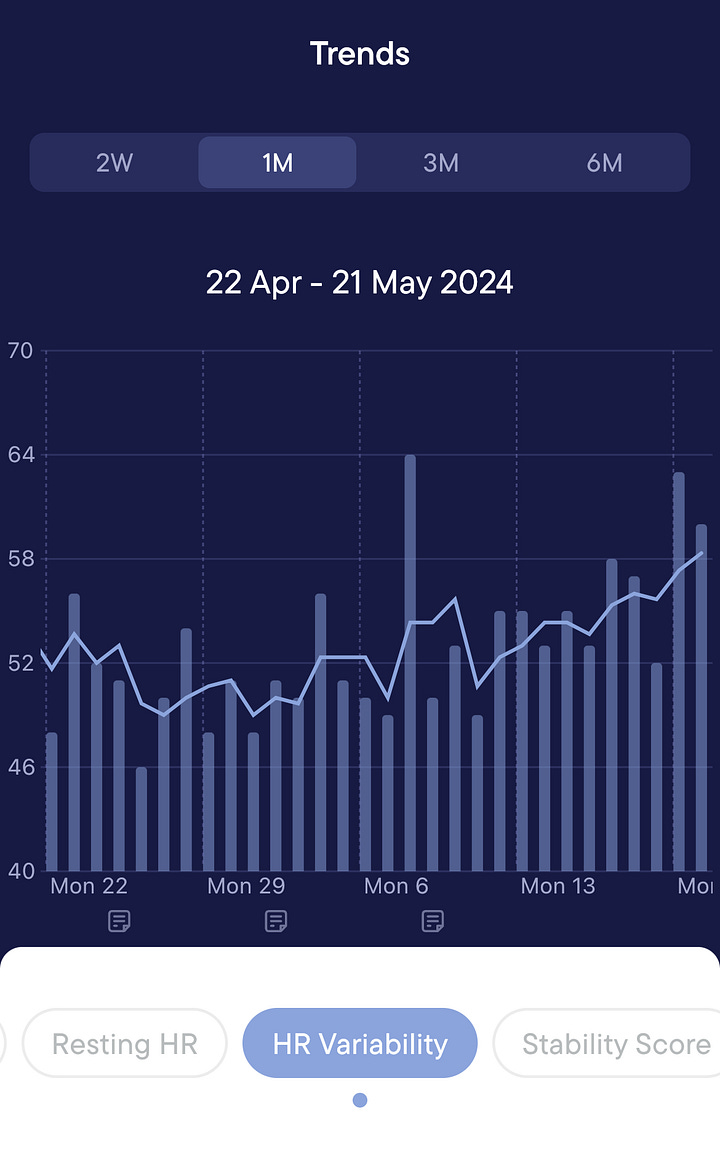
Three years later, a fresh set of eyes and a NASA lean test—I’ve got POTS (extremely common with ME)! Maybe it was missed on the tilt table test in ‘21 or maybe it since developed. But having a thorough, engaged and invested doctor telling me treatment is imperative was enough to get me to commit. A lot of you probably already know this, but dealing with POTS is seriously a full-time job! And, frankly, the job sucks. But the improvement was nearly immediate and substantial. Floating through the day on 3+ liters of fluids, calculating my grams of sodium every day, strapping in and out of abdominal compression, strategizing time to sit and recline—it’s A LOT but totally worth it. I’ve also been put on Guanfacine, which has reduced my heart rate throughout the day, giving me a very nice boost to my baseline by expanding my energy envelope. There are a lot of options for managing POTS with medication, this one happens to be working for me right now.
The other major addition to my treatment plan is Low Dose Abilify (LDA), which has grown to be pretty legendary in the ME community (read Whitney Dafoe’s experience). I won’t get into the mechanism of how they believe it works and the differences between the “regular” dose vs. the low dose used for ME, you can check that out here—it’s very cool. For anyone who doesn’t believe or understand that ME is a disease of the brain and nervous system, they need to look closely at the drugs and doses that work for us—there’s no denying it!
Disclaimer! We are an incredibly heterogeneous group. There are tons of strings being pulled with this disease, so there’s lots of room for medication reactions. Not everyone responds to drugs the same way, positively or negatively. It’s a frustrating trial and error but that’s where we’re at.
I started LDA at 0.5mg. I received 2mg tablets and used a pill cutter. Within a few days, I started getting migraines. As they got worse and I found it intolerable, I stopped the LDA, and the migraines stopped. So, I took to the pill cutter and got down to 0.25mg. Success! No migraines and within about a week I could tell the drug was having an effect. I stayed at that dose for two months before trying 0.5 again. I’ve now been at 0.5mg for a few weeks with success. LDA works for us at different doses anywhere between 0.1-2mg. The goal is not to get to 2mg at all costs. The goal is to find the dose that measurably works for you and hold. This appears to be a drug that often stops working for us over time, so having room to move up on your dose through time can be helpful.
We’ve made a few smaller adjustments as well, like increasing my LDN (low does naltrexone), switching to a different antiviral, adding an H2 inhibitor to my other mast cell stabilizers and dialing in my supplements. Separately, my immunologist is changing my immunoglobulin replacement therapy from subcutaneous to intravenous, in the hopes that it can more effectively deal with the immune dysfunction in addition to my immune deficiency. It’s been a busy and slightly overwhelming year so far! I sat on a four-month waiting list to get into this new ME doctor and it was absolutely worth it (a short wait compared to others).
If I could gift our community anything, it would be access to medical treatment. This level of care is transformative and possibly lifesaving. This is why MEAction’s current campaign, Teach ME Treat ME, is so crucial. In addition to sharing the remote providers I’m aware of above, I want to share the supplement and therapy recommendations I’ve received from my ME doctor. These are things that don’t require prescriptions, so if your budget allows, you might find some relief.
This is not medical advice. I’m only sharing my experience.
Ubiquinol: antioxidant/neuroinflammation, 200 - 600 mg in the morning
Alpha Lipoic Acid: antioxidant/mast cell stabilizer, up to 250 mg 3x a day
N-Acetyl Cystine: antioxidant/produces glutathione, 500 mg 2x a day
Curcumin: antioxidant/crosses blood brain barrier, 1500 mg 1x a day
Vitamin B complex & vitamin D: dose based on blood work
Pepcid: H2 inhibitor/mast cell stabilizer, 20 mg 2x a day
Dextromethorphan (common cough suppressant): neuroinflammation/pain, 15 mg 3x a day, trial for two weeks to see if you respond with symptom improvement, if not stop taking
Saccharomyces boulardii (yeast): microbiome/mast cell stabilizer, 1 capsule daily
Vagus Nerve Stimulation Therapy: I use Truvaga, there are several options
Red Light/Near Infared Therapy: I use Hooga, there are many options
Compression Leg Sleeves: circulation/orthostatic intolerance, ReAthlete is one of many options
Hydraulic Eye Massager (not a recommendation from doc, but I find this helps with sleep and headaches)
For what it’s worth, that’s my current list! There’s a never-ending list of potential supplements, therapies and medications floating around the community all the time. Some may help, others won’t. It can get difficult to tell what’s doing what. I recommend keeping a calendar, starting with one at a time and giving it at least two weeks. Note any changes, decide to keep going or stop and then introduce something else. It takes forever, but it’s really helpful. Not everything will produce a noticeable effect, so if you feel strongly about the research behind it but don’t feel any change, I say keep taking it.
Do what you can, when you can. Don’t make yourself stressed. Be systematic. Go slow. Have patience and give yourself permission to pause. This thing we call “treatment” is imperfect and that isn’t our fault. It’s a deep failing beyond our control.



I just started radical rest myself to see if that will help me reverse my progression into severe. I hope yours has helped you. Thanks for posting--it's nice knowing I'm not alone.
I recommend Center for Complex Diseases, Dr David Kaufman (also sees patients remotely). Also listed on MEAction’s list of ME competent doctors. He has been super helpful for my Long Covid, after 4 years of struggle.